Biomarker for Inflammatory Bowel Disease
Background
Inflammatory Bowel Disease (IBD) includes Crohn’s Disease and ulcerative colitis (UC). There is no definitive test for diagnosing IBD and its diagnosis involves a number of invasive tests such as colonoscopies, biopsies and blood tests. Tests that screen for fecal inflammatory biomarkers and serological markers are in development. Given that IBD is a heterogeneous disease and subsets of patients may be defined by genetic and subclinical markers that reflect specific types of inflammation, each IBD subtype represents an opportunity for individualized treatment approaches. Therefore additional biomarkers that may be added to the panel of biomarkers to improve the diagnosis of IBD are essential.
Brief Description
Prof. Declan McCole and his colleagues at the University of California, Riverside have identified that increased levels of carcinoembryonic antigen-related cell adhesion molecule 6 (CEACAM6) correlate to a loss of function mutation in a protein tyrosine phosphatase non-receptor type 2 (PTPN2) gene. PTPN2 has been identified as an IBD candidate gene that protects the intestinal epithelial barrier. Dysfunction of the PTPN2 gene, which encodes the T-cell protein tyrosine phosphatase (TCPTP) protein, contributes to alterations in the intestinal microbiome and the onset of chronic intestinal inflammation which is a symptom of IBD. Loss of function of PTPN2 has resulted in IBD-like symptoms in mice and caused the increased abundance of the intestinal pathobiont adherent-invasive Escherichia coli that binds to CEACAM6 and increases a patient’s susceptibility to IBD.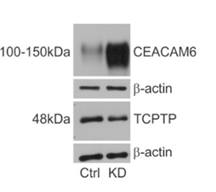
Fig. 1 shows control and PTPN2-KD cell lysates with reduced protein expression of TCPTP (PTPN2) in PTPN2-deficient cells that express increased CEACAM6 protein when compared to control cells
Suggested uses
- The diagnosis of IBD using CEACAM6 as a biomarker to correlate to loss of PTPN2 activity.
Patent Status
| Country | Type | Number | Dated | Case |
| United States Of America | Issued Patent | 11,150,237 | 10/19/2021 | 2018-548 |
Contact
- Grace Yee
- grace.yee@ucr.edu
- tel: View Phone Number.
Other Information
Keywords
inflammatory bowel disease, IBD, biomarker, Crohn's Disease, ulcerative colitis, CEACAM6, PTPN2, TCPTP
